Women between the ages of 50 and 70 and who are insured with the CNS are automatically invited to get a mammogram. Men, who account for less than 1% of breast cancer aren’t targeted by these campaigns. Women under 50, even though they represent registered in the EU--aren’t either.
For the health ministry, mass invitations to scans isn’t the solution--training doctors to recognise the symptoms is.
Rare but there
The fact that men and young women represent minorities means little awareness is raised around the subject.
“We always talk about breast cancer being possible in both men and women and usually add that about 1% of new cases of breast cancer will be in men,” a spokesperson for breast cancer awareness association Think Pink Luxembourg tells Delano. “With young women, we let them know that it is something that affects them.”
About 1% of new cases of breast cancer will be in men.
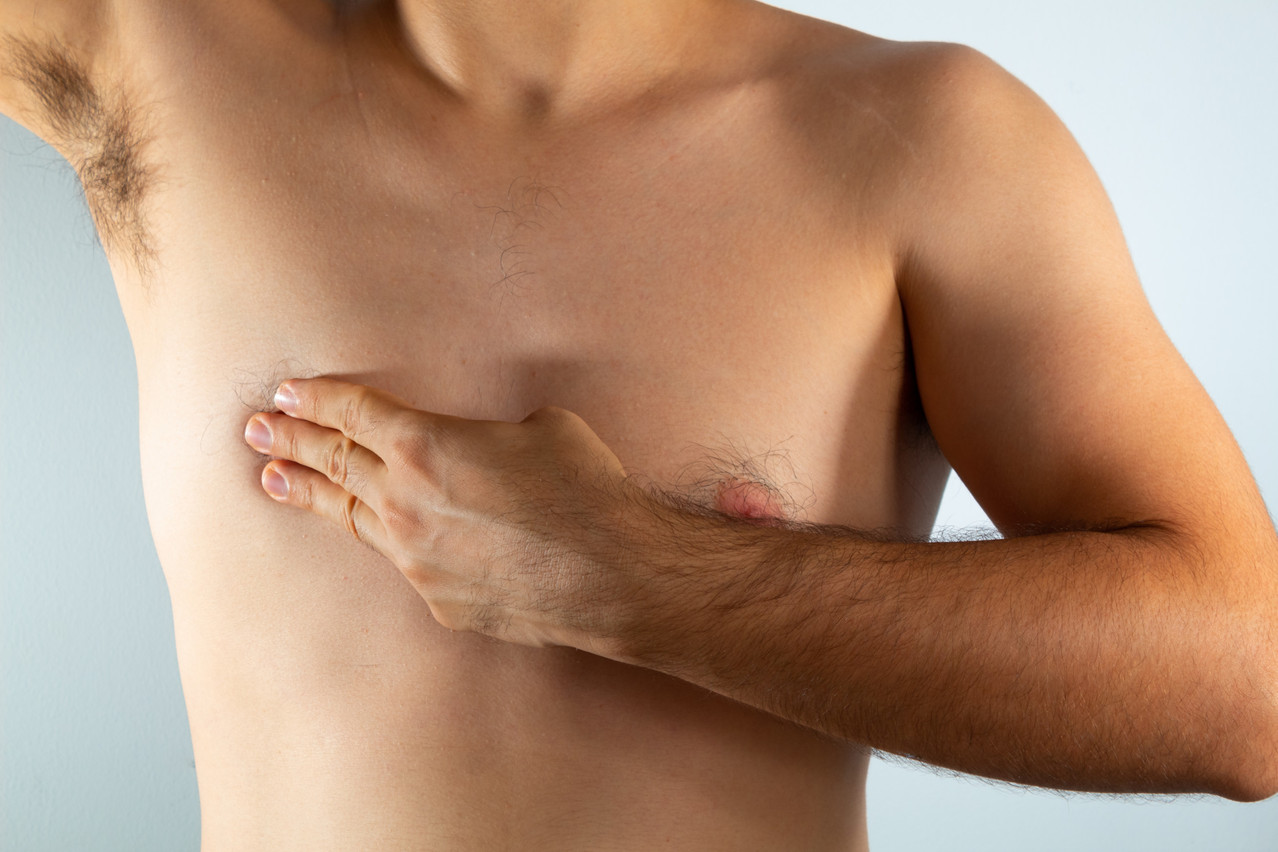
Symptoms of breast cancer in both groups are the same as for women between 50 and 70: for most, a lump that feels like a hard knot or a thickening will appear in the breast or under the arm and not disappear on its own. Irregularities on the skin or nipple can also be indicators: redness, scaliness, puckering, or a discharge from the nipple are also signs that something isn’t right.
Understanding male breast cancer
“Male breast cancers are often misunderstood,” . This can lead to inadequate treatment and a higher mortality rate.
Without a significant local pool of participants to rely on, global experts from Northern America and Europe in 2006 launched the long-term programme, in an effort to better grasp the pathologic specificities found in men.
They found that “several genetic disorders (e.g. Kleinefelter’s syndrome) can increase the risk of the disease by 50-fold. A family history of breast and ovarian cancer is reported in approximately 15%–20% of men with BC [breast cancer].”
Low testosterone and high estrogen can also lead to the development of breast cancer in men. Black men are more than twice more likely to develop the illness than Caucasians, according to the health ministry.
Uncoupling breast cancer from gender
Mammographies and echographies are used to diagnose breast cancer in men, as the CHL’s confirms. Every year, around 80 to 100 men undergo the imaging procedure, says health minister Paulette Lenert’s
“The process is pretty much the same for men as for women,” the CHL’s specialised said in an interview with Delano. Like women, treatment for men involves chemotherapy coupled with a mastectomy if necessary.
Read also
But for the health ministry, an automatic screening of all men isn’t justified due to the low incidence. “In fact, breast cancer screening for all men would have no effect on breast cancer mortality and would result in a very high number of unnecessary examinations.” In a country where women outside the usual scope can wait up to 18 months for an appointment, this appears justified.
Either way “men are usually screened for colon or prostate cancers--so usually they’ll have found a lump themselves and gone for an exam,” Benoist continues. Some men might associate this type of cancer with women, she says, so don’t necessarily connect the dots when symptoms show up.
Outside the scope
Only 5% of breast cancers in Luxembourg affect women under the age of 35--often because of familial inheritance--but when they occur, they are more aggressive and develop rapidly. Including younger women in the scope of its mammography programme would create too large a demand, the ministry explains. Plus, the exposure to X-rays during these exams causes more harm to younger breast tissue. This, for the ministry, is an argument not to extend the scope of the national mammography programme.
For young women, rather than the exclusion from awareness campaigns, the long waiting period between initial suspicions and mammography appointments can be an issue.
“Sometimes young patients only get an appointment a year after requesting one,” Benoist explains. “This is more problematic than the prevention efforts,” which she says are great especially around Pink October.
The other difficulty lies in reading the results of a mammography as the density of the breast tissue fluctuates a lot in women who have not yet reached menopause.
Efficient prevention over aimless testing
So the issue is two-fold: on the field, the need for increasing operations to meet demands is clear. “They just need to make more time available. There are so many women who have to undergo the exam every two years, so there should be more slots, of which some would be kept free for these kinds of emergencies,” says Benoist. But most emergency appointments between 2019 and 2022 just took a week of waiting, , meaning that the issue, for the ministry lies elsewhere.
Read also
Indeed, the health ministry says that general practitioners and gynaecologists also have a role to play in detecting the cancer. Rather than looking to increase the scope of mammography invitations, it wants to push doctors to better recognise suspicious cases. To complement that, self-examinations can help.
Ultimately, as Benoist stresses, “what’s important, is that if you feel something in your breast, you shouldn’t leave it aside. It can sometimes be a hormonal lump but sometimes not.” And this is true regardless of age and gender.